

The effects of climate change are becoming increasingly severe, and climate-driven health challenges are becoming increasingly prevalent. Malaria is no exception to this trend. A preventable and climate-sensitive disease, malaria is the cause of over 600,000 deaths worldwide every year — 96% of whom live in Africa and 75% of whom are children under five years old — and that number is only expected to grow with the evolving state of climate change. In Nigeria, where Dr. Unwana Usoro (image below) practices, these effects are only becoming more and more apparent.
The climate-malaria nexus emphasizes the urgent need to build resilient systems and communities that can adapt to this evolving threat in eradicating malaria. Highlighting the interconnectedness of climate change and malaria sheds light on the importance of social and behavioral change programs and other innovative solutions to mitigate its impact.

The climate-malaria nexus is a multifaceted challenge, as climate change affects a range of factors such as temperature, humidity, and rainfall, each of which impacts malaria transmission differently.
Climate change is causing the range of malaria-carrying mosquitoes to expand, bringing the disease to new regions that were once considered low-risk. For example, the Andes Mountains in Colombia, Peru, and Ecuador, previously regarded as low-risk areas, are now experiencing longer transmission periods, nearly double what they had before 2000. Changes in rainfall patterns, linked to climate change, have also created more breeding sites for malaria-transmitting mosquitoes. In Kenya, intense flooding resulting from climate change has led to a surge in malaria cases after a period of severe drought. Climate-induced factors like rainfall and humidity help create ideal conditions for mosquito breeding and malaria transmission in regions previously deemed low-risk.

Furthermore, climate change has expanded the geographical range of malaria transmission in sub-Saharan Africa, with mosquitoes and the disease spreading to higher altitudes each year. This phenomenon is driven by the faster reproduction of mosquitoes and the parasites they carry in warmer temperatures. The movements of human populations and changes in land use also contribute to the disease’s expansion.
In addition to these changes, African nations are now facing a new threat from the Anopheles stephensi mosquito, which is well adapted to urban environments and has the potential to expose an additional millions of people to malaria. This mosquito species arrived in Africa in 2012 and has since spread through several countries, including Kenya, where its proliferation is likely influenced by changing climate patterns.
Needless to say, to combat this alarming trend that’s overwhelming health systems across the globe, we must continuously adopt multi-faceted approaches and prioritize building resilient and sustainable systems for this global health challenge. Malaria is a global challenge that transcends borders and requires coordinated efforts.
“For [malaria] prevention, I think using a combination of measures rather than any one is ideally needed.” —Dr. Usoro

Social and behavioral change (SBC) plays a pivotal role in educating communities about the implications of climate change on malaria and how individual actions can contribute to its spread or prevention. The Fighting Malaria with Social and Behavior Change (FMSBC) program funded by USAID in Mozambique is currently exploring this. The program employs a human-centered design (HCD) approach, involving NGO partners in activities aimed at self-assessment and identifying their own skill gaps. These partners then tailor interventions to align more closely with the specific needs of their target communities. Outreach campaigns utilize various mediums, including radio broadcasts, traditional advertising, and innovative community-based approaches to disseminate critical messages for behavior change.
In low-risk areas, educational initiatives can specifically help people recognize the risks associated with climate change, adapt to potential new challenges, and become active participants in malaria prevention. Community members can identify potential breeding sites better than outsider researchers, and take preventive measures within their own homes, such as draining stagnant water, closing doors early, and cutting excess greenery.
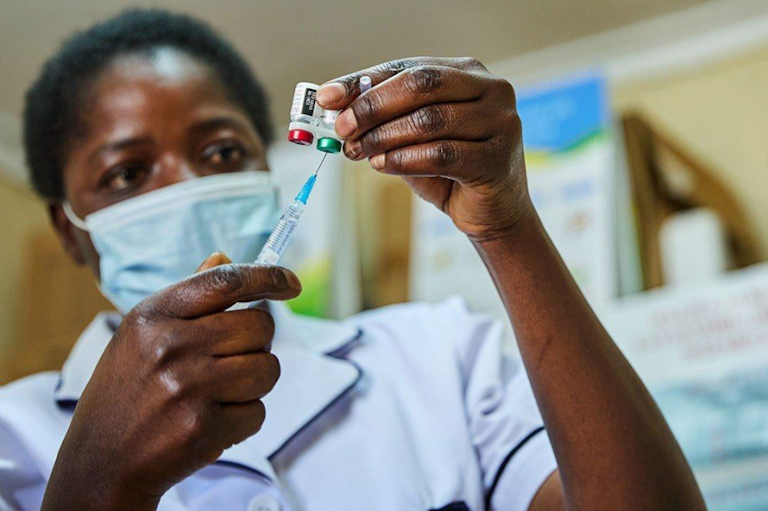
An obvious noteworthy approach to tackling malaria is the WHO recommendation of two new vaccines. Approved for use in regions with moderate to high P. falciparum malaria transmission, the pioneering RTS,S/AS01 vaccine has been shown to significantly reduce malaria, and deadly severe malaria, among young children; and the second WHO-endorsed malaria vaccine — R21/Matrix-M — has shown to be similarly effective in large-scale trials. These two breakthroughs offer hope in preventing new malaria cases, especially in regions where climate change is exacerbating its transmission. If and when widely accessible, the vaccine could save countless lives and serve as an essential tool in building resilience against climate-driven malaria.
“The malaria vaccines would definitely be a much-needed help in mitigating disease burden here, being that it is an endemic region. Unfortunately, Nigeria does not have access to any of the vaccines currently, so there are no programs for its administration … We aim to prevent future cases through patient education. This is communicated verbally most times, in English and Pidgin English which are widely spoken in Nigeria. We inform them about malaria, how it presents, preventive measures, and the importance of treatment.” — Dr. Usoro
However, the fight against climate-driven malaria goes beyond these individual actions; it requires systemic changes. Traditional systems of addressing the disease are no longer adequate, calling for a radical shift in our thinking. To build resilient systems and communities that can effectively combat climate-driven malaria, we must consider more novel solutions. It involves reimagining healthcare systems, integrating climate data into public health policies and surveillance, and engaging in interdisciplinary research and collaboration. By adopting a holistic approach that combines the expertise of climate scientists, health professionals, and community leaders, we can create more robust systems that are better equipped to address the challenges posed by a changing climate.
Experts are increasingly using urgent language to describe the state of climate change, and our responsibility to address it head-on. The climate-malaria nexus presents an urgent call to action for building resilient systems and communities that can adapt to the ever-evolving challenges of our warming globe. The development of the new vaccine and provision of SBC techniques provides hope, but our long-term success depends on our collective ability to think creatively and act decisively in the face of this complex, climate-driven health crisis.
Ezinwa Osuoha is a Master’s in Public Health student at the Yale School of Public Health, a fellow at the United States Agency for International Development, and a United to Beat Malaria College Ambassador. Passionate about global health and international policy, her interests encompass the environmental, social, and behavioral factors of disease transmission.
Visit beatmalaria.org/climate to hear more perspectives about climate change’s impact on malaria and solutions to make malaria programs more climate resilient.